Not all sedation is created equal — and understanding the difference can make all the difference for your patients.
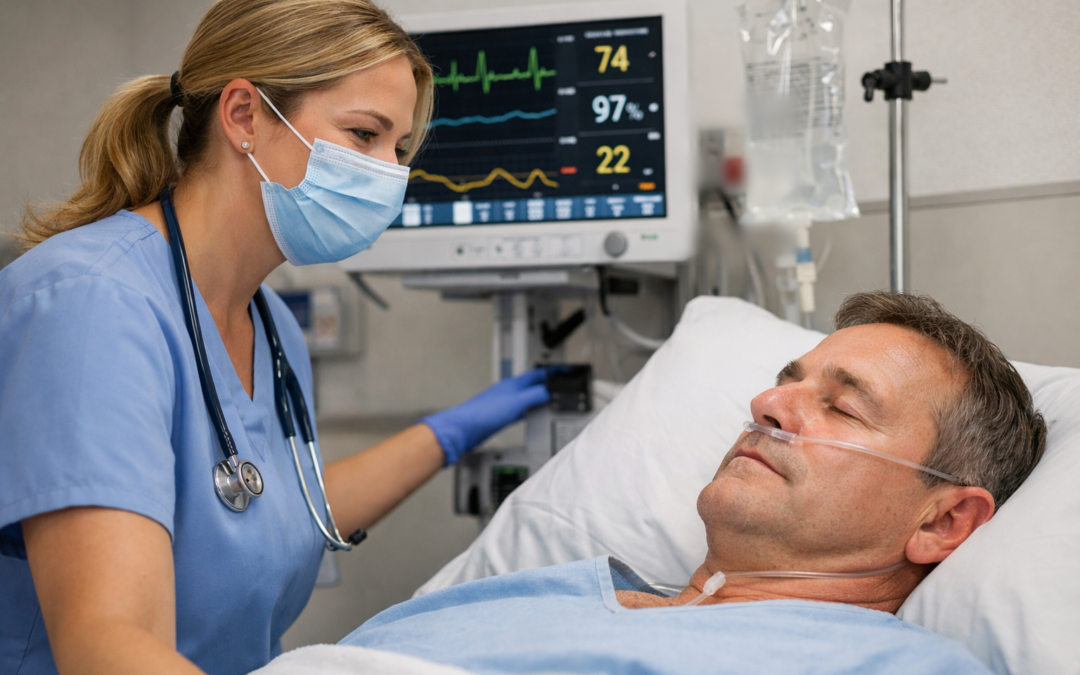
If you work in procedural sedation outside of the operating room, you already know that preparation is everything. But one of the most foundational concepts — and one that still causes confusion in clinical settings — is the difference between minimal and moderate sedation. Understanding these sedation levels, how your patient should respond, and what monitoring is required isn’t just good practice. It is essential for patient safety.
Let’s break it down together.
The Sedation Continuum: A Quick Overview
Sedation exists on a continuum. The American Society of Anesthesiologists (ASA) defines four distinct levels: minimal sedation (anxiolysis), moderate sedation/analgesia, deep sedation, and general anesthesia. Each level is defined by how deeply the patient is affected — and critically, each carries its own expectations for patient responsiveness, airway management, and monitoring requirements.
For non-anesthesia providers, the two most commonly administered levels are minimal sedation and moderate sedation. Knowing exactly where your patient falls on that continuum — and being prepared if they drift deeper — is what separates a safe procedure from a dangerous one.
Minimal Sedation: Alert, Calm, and Cooperative
Minimal sedation, also called anxiolysis, is exactly what it sounds like: a light touch. At this level, patients respond normally to verbal commands. Their cognitive function and coordination may be mildly impaired, but their airway reflexes, ventilation, and cardiovascular function remain completely unaffected.
Think of it as taking the edge off. A patient who is anxious about a procedure can be calmed without losing awareness or protective reflexes. Common examples include the administration of low-dose oral benzodiazepines or nitrous oxide before a dental or diagnostic procedure.
Moderate Sedation: Purposeful, Not Absent
Moderate sedation — sometimes called procedural sedation or conscious sedation — is a step deeper. At this level, patients experience a depression of consciousness, but they can still respond purposefully to verbal commands or light tactile stimulation. That word “purposefully” matters. Reflex withdrawal from a painful stimulus does not count as a purposeful response.
The patient’s airway remains patent and self-maintained, spontaneous ventilation is adequate, and cardiovascular function is usually well preserved. This is the level most commonly used for GI endoscopies, cardiac catheterizations, minor surgical procedures, and various diagnostic interventions.
Side-by-Side: Minimal vs. Moderate Sedation
| Feature | Minimal Sedation | Moderate Sedation |
|---|---|---|
| Responsiveness | Normal response to verbal commands | Purposeful response to verbal or tactile stimulation |
| Airway | Unaffected | No intervention required |
| Spontaneous Ventilation | Unaffected | Adequate |
| Cardiovascular Function | Unaffected | Usually maintained |
| Monitoring Requirements | Baseline vitals; periodic reassessment | Continuous SpO₂, HR, RR, BP, and level of consciousness |
| Dedicated Monitor Required | Not always required | Yes — the monitoring clinician should not also perform the procedure |
Sedation Monitoring: Why It Matters So Much
One of the most critical — and sometimes misunderstood — aspects of sedation administration is monitoring. For moderate sedation, continuous monitoring is non-negotiable. This includes oxygen saturation (SpO₂) via pulse oximetry, heart rate and rhythm, respiratory rate, blood pressure at regular intervals, and ongoing assessment of the patient’s level of consciousness throughout the procedure.
Equally important is having a qualified individual whose sole responsibility is watching the patient — someone who is not also performing the procedure. This standard, reinforced by The Joint Commission and institutional policies nationwide, exists because sedated patients can change quickly, and a divided focus can lead to missed warning signs.
Capnography (end-tidal CO₂ monitoring) is also increasingly recommended for moderate sedation, providing an early warning of respiratory depression before oxygen saturation even begins to drop.
The Risk of Unintended Deeper Sedation
Here is something every sedation provider needs to understand: sedation levels are not static. A patient who appears to be in moderate sedation can quickly drift into deep sedation — especially with repeated dosing, in elderly patients, or in those with underlying medical conditions.
That is why providers administering moderate sedation must be trained to recognize deeper sedation and be prepared to manage it. This means knowing how to maintain a patent airway, support ventilation, and respond quickly when a patient is no longer arousable.
Training doesn’t just reduce risk — it builds the confidence and competence your patients deserve.
Ready to Strengthen Your Sedation Practice?
Whether you’re new to procedural sedation or looking to recertify, the National Sedation Center offers comprehensive, evidence-based courses designed specifically for non-anesthesia healthcare providers. Our curriculum covers sedation levels, monitoring standards, patient assessment, and emergency preparedness — everything you need to practice with confidence.